Hemorrhoids
Did you know…
Hemorrhoids are one of the most common ailments known.
- More than half the population will develop hemorrhoids, usually after age 30.
- Millions of Americans currently suffer from hemorrhoids.
- The average person suffers in silence for a long period before seeking medical care.
- Today’s treatment methods make some types of hemorrhoid removal much less painful.
What are hemorrhoids?
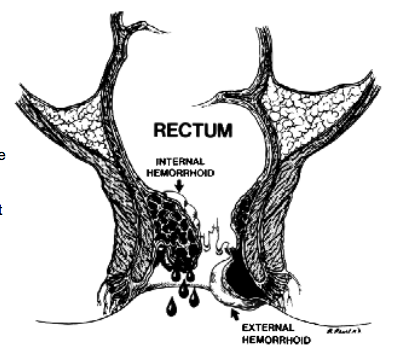
Often described as “varicose veins of the anus and rectum”, hemorrhoids are enlarged, bulging blood vessels in and about the anus and lower rectum. There are two types of hemorrhoids: external and internal, which refer to their location.
External (outside) hemorrhoids develop near the anus and are covered by very sensitive skin. These are usually painless. However, if a blood clot (thrombosis) develops in an external hemorrhoid, it becomes a painful, hard lump. The external hemorrhoid may bleed if it ruptures.
Internal (inside) hemorrhoids develop within the anus beneath the lining. Painless bleeding and protrusion during bowel movements are the most common symptom. However, an internal hemorrhoid can cause severe pain if it is completely “prolapsed” – protrudes from the anal opening and cannot be pushed back inside.
What causes hemorrhoids?
An exact cause is unknown; however, the upright posture of humans alone forces a great deal of pressure on the rectal veins, which sometimes causes them to bulge.
Other contributing factors include:
- Aging
- Chronic constipation or diarrhea
- Pregnancy
- Heredity
- Straining during bowel movements
- Faulty bowel function due to overuse of laxatives or enemas
- Spending long periods of time (e.g., reading) on the toilet
Whatever the cause, the tissues supporting the vessels stretch. As a result, the vessels dilate; their walls become thin and bleed. If the stretching and pressure continue, the weakened vessels protrude.
What are the symptoms?
If you notice any of the following, you could have hemorrhoids:
- Bleeding during bowel movements
- Protrusion during bowel movements
- Itching in the anal area
- Pain
- Sensitive lump(s)
How are hemorrhoids treated?
Mild symptoms can be relieved frequently by increasing the amount of fiber (e.g., fruits, vegetables, breads and cereals) and fluids in the diet. Eliminating excessive straining reduces the pressure on hemorrhoids and helps prevent them from protruding. A sitz bath – sitting in plain warm water for about 10 minutes – can also provide some relief .
With these measures, the pain and swelling of most symptomatic hemorrhoids will decrease in two to seven days, and the firm lump should recede within four to six weeks. In cases of severe or persistent pain from a thrombosed hemorrhoid, your physician may elect to remove the hemorrhoid containing the clot with a small incision. Performed under local anesthesia as an outpatient, this procedure generally provides relief.
Severe hemorrhoids may require special treatment, much of which can be performed on an outpatient basis.
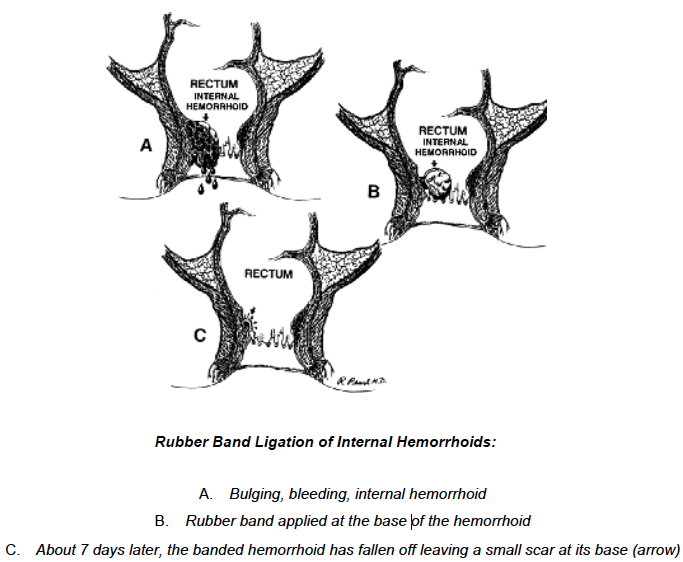
Ligation – the rubber band treatment – works effectively on internal hemorrhoids that protrude with bowel movements. A small rubber band is placed over the hemorrhoid, cutting off its blood supply. The hemorrhoid and the band fall off in a few days and the wound usually heals in a week or two. This procedure sometimes produces mild discomfort and bleeding and may need to be repeated for a full effect.
Injection and Coagulation can also be used on bleeding hemorrhoids that do not protrude. Both methods are relatively painless and cause the hemorrhoid to shrivel up.
Hemorrhoid stapling – this is a technique that uses a special device to internally staple and excise internal hemorrhoidal tissue. The stapling method may lead to shrinkage of but does not remove external hemorrhoids. This procedure is generally more painful that rubber band ligation and less painful than hemorroidectomy.
Hemorrhoidectomy – surgery to remove the hemorrhoids – is the most complete method for removal of internal and external hemorrhoids. It is necessary when (1) clots repeatedly form in external hemorrhoids; (2) ligation fails to treat internal hemorrhoids; (3) the protruding hemorrhoid cannot be reduced; or (4) there is persistent bleeding. A hemorrhoidectomy removes excessive tissue that causes the bleeding and protrusion. It is done under anesthesia using either sutures or staplers, and may, depending upon circumstances, require hospitalization and a period of inactivity. Laser hemorrhoidectomies do not offer any advantage over standard operative techniques. They are also quite expensive, and contrary to popular belief, are no less painful. Rubber Band Ligation of Internal Hemorrhoids: A. Bulging, bleeding, internal hemorrhoid B. Rubber band applied at the base of the hemorrhoid C. About 7 days later, the banded hemorrhoid has fallen off leaving a small scar at its base (arrow)
Do hemorrhoids lead to cancer?
No. There is no relationship between hemorrhoids and cancer. However, the symptoms of hemorrhoids, particularly bleeding, are similar to those of colorectal cancer and other diseases of the digestive system. Therefore, it is important that all symptoms are investigated by a physician specially trained in treating diseases of the colon and rectum and that everyone 50 years or older undergo screening tests for colorectal cancer. Do not rely on over-the-counter medications or other self-treatments. See a colorectal surgeon first so your symptoms can be properly evaluated and effective treatment prescribed.